
Key Takeaways
- Bipolar disorder and borderline personality disorder (BPD) may share some symptoms, but they are fundamentally different.
- BPD is a personality disorder marked by rapid emotional changes, while bipolar disorder is a mood disorder with longer-lasting episodes of mania or depression.
- BPD causes rapid mood changes triggered by stress or relationships, while bipolar disorder involves longer mood episodes of mania and depression.
- BPD is mainly treated with therapy, while bipolar disorder usually needs medication plus therapy.
However, these are two distinct conditions. BPD is associated with persistent emotional instability, where emotions can change rapidly in response to everyday events. Bipolar disorder, on the other hand, involves longer-lasting mood episodes, cycling between periods of depression and mania or hypomania.
In this blog, we’ll explore the key differences between borderline personality disorder and bipolar disorder. We’ll break down the symptoms that make them look so alike, explain what actually sets them apart, and walk through how each condition is diagnosed and treated.
What Is Borderline Personality Disorder (BPD)?
Borderline personality disorder (BPD) is a mental health condition that affects how a person manages emotions, sees themselves, and interacts with others. It is not just moodiness; it is a deeply rooted pattern that can affect nearly every area of someone’s life. Research suggests that about 1.6% of the population in the United States lives with BPD, showing that this condition is more common than many people realize.
People with borderline personality disorder (BPD) often experience rapid and strong mood changes, which can be triggered by everyday situations, especially in relationships. These emotional shifts may lead to feelings of anger, sadness, anxiety, or emptiness that can be difficult to control.
Furthermore, those living with this condition often experience higher rates of comorbidity. This means they may also have other mental health conditions at the same time, such as depression, anxiety disorders, PTSD, substance use disorders, or eating disorders.
Symptoms of BPD
People with BPD often experience a range of challenging symptoms. The most common ones include:
• Intense fear of abandonment, even when there is no real threat of it.
• Unstable relationships that swing between idealization and intense anger.
• Mood swings that shift within hours, often triggered by interpersonal events.
• Impulsive behaviors such as risky spending, substance use, or reckless actions.
• Chronic feelings of emptiness.
• Self-harm or suicidal behavior, especially during emotional crises.
• Brief episodes of paranoia or dissociation under stress.
What Causes Borderline Personality Disorder
BPD doesn’t have one clear cause. Researchers believe it likely arises from a combination of factors, including genetic vulnerability, neurobiological differences, and early life experiences.
Many people with BPD have a history of childhood trauma, emotional neglect, or invalidation. However, trauma alone does not cause BPD. Additionally, temperament also plays a significant role. Some people are simply born with a more sensitive emotional system, and when that sensitivity meets a difficult environment, BPD can develop.
Treatment for BPD
Psychotherapy (talk therapy) is the primary treatment for BPD. The aim of therapy is to reduce emotional instability, suicidal behavior, and impulsivity. There are different types of talk therapy that can help, including:
- Dialectical Behavior Therapy (DBT): Focuses on emotional regulation, mindfulness, and coping skills.
- Cognitive Behavioral Therapy (CBT): Helps identify and change negative thought patterns and behaviors.
- Schema-Focused Therapy: Addresses deep-seated patterns and beliefs formed in early life.
- Mentalization-Based Therapy (MBT): Improves understanding of one’s own and others’ thoughts and feelings.
- Transference-Focused Psychotherapy (TFP): Explores interpersonal relationships and emotional experiences to improve behavior.
Now, let’s explore bipolar disorder and see what sets it apart from BPD, focusing on the key differences in bipolar disorder vs bpd.
What Is Bipolar Disorder?
Bipolar disorder is a mental health condition that causes extreme mood swings, including emotional highs (mania or hypomania) and lows (depression). These shifts can affect how people think, feel, and behave, which makes daily life challenging. In the United States, it affects approximately 5.7 million adults, or about 2.6% of the population, showing how common this condition is.
During manic or hypomanic episodes, a person may feel unusually energetic, euphoric, or irritable. They might take risks, talk quickly, or have racing thoughts. On the other hand, during depressive episodes, a person may feel sad, hopeless, or exhausted, lose interest in activities, struggle to concentrate, or have changes in sleep and appetite.
Types of Bipolar Disorder
Bipolar disorder can take different forms, each with unique patterns of mood episodes:
- Bipolar I Disorder: It Involves at least one full manic episode, often accompanied by periods of depression.
- Bipolar II Disorder: It is characterized by hypomanic episodes (which are less severe than full mania) and episodes of major depression.
- Cyclothymic Disorder: Milder mood swings that last for at least two years, with periods of hypomania and mild depression.
Symptoms of Bipolar Disorder
1. Manic or Hypomanic Symptoms:
- Feeling extremely energetic, euphoric, or unusually irritable.
- Racing thoughts and rapid speech.
- Increased activity or restlessness.
- Impulsive or risky behavior.
- Reduced need for sleep.
- Inflated self-esteem or grandiosity.
2. Depressive Symptoms:
- Persistent sadness or hopelessness.
- Loss of interest or pleasure in activities once enjoyed.
- Fatigue or low energy.
- Difficulty concentrating or making decisions.
- Changes in sleep patterns (sleeping too much or too little).
- Changes in appetite or weight.
- Feelings of worthlessness or excessive guilt.
- Thoughts of death or suicidal behavior.
3. Other Possible Symptoms:
- Anxiety or agitation.
- Irritability or mood swings between episodes.
- Difficulty maintaining relationships or daily responsibilities.
Treatment
Medication is the foundation of treatment for bipolar disorder. Psychotherapy plays an important supporting role, but mood stabilization with medication typically comes first.
- Medications: Bipolar disorder is often treated with medications to stabilize mood. Common options include mood stabilizers, antidepressants, and antipsychotics to help manage episodes of mania, hypomania, and depression.
- Psychotherapy: Therapy is also important for bipolar disorder, but the focus differs from BPD. Therapies like cognitive behavioral therapy (CBT), interpersonal and social rhythm therapy (IPSRT), and family-focused therapy help individuals understand mood patterns, cope with symptoms, and maintain stable daily routines.
- Lifestyle and Support: Regular sleep, stress management, avoiding alcohol or drugs, and having a supportive environment are also important for long-term stability in bipolar disorder.
Helping Children Find Emotional Balance
Join a clinical study exploring new approaches to managing pediatric bipolar disorder.
While talk therapy is the main treatment for BPD, bipolar disorder often requires a combination of medication and therapy to manage the cyclical mood episodes.
What’s the Difference Between BPD and Bipolar Disorder: Side-by-Side Comparison
| Feature | Bipolar Disorder | Borderline Personality Disorder (BPD) |
|---|---|---|
| Condition type | Mood disorder | Personality disorder |
| Mood episode length | Days to months | Hours to days |
| Triggers | Can occur with or without clear external triggers | Usually triggered by interpersonal stress or events |
| Self-image | Stable between episodes | Chronically unstable |
| Trauma link | Less direct | Strong, especially early childhood |
| Primary treatment | Medication + therapy | Psychotherapy (DBT) first |
Bipolar VS Borderline Personality Disorder: Overlapping Symptoms
Even though BPD and bipolar disorder are distinct conditions, they share some symptoms, which is why confusion can occur. This visual highlights both the overlaps and the differences:
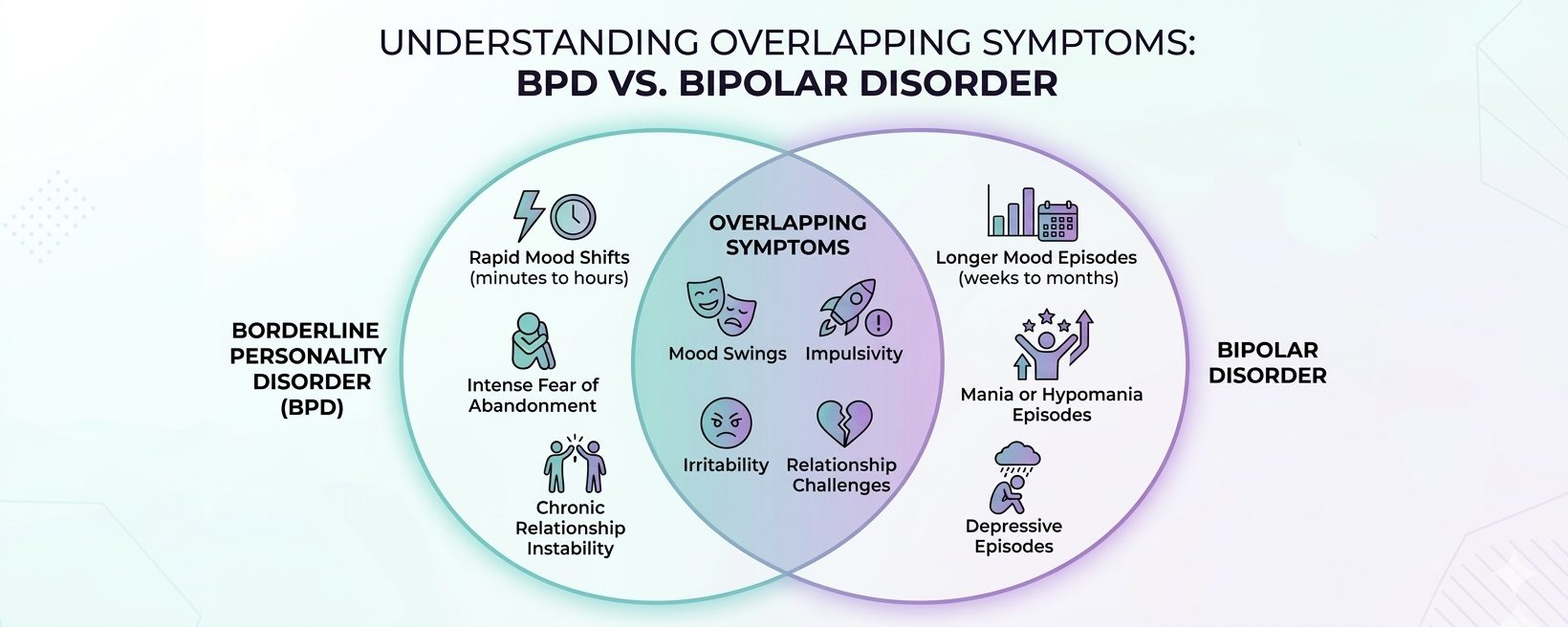
These overlapping symptoms can make it challenging to tell the two conditions apart. However, by understanding both the shared and unique traits, it becomes easier to recognize each condition and guide proper support or treatment.
Can You Have Both BPD and Bipolar Disorder at the Same Time?
Yes, it is possible for someone to experience both borderline personality disorder (BPD) and bipolar disorder at the same time. In fact, research shows that about 20% of people with bipolar disorder also have borderline personality disorder.
This overlap is an important consideration in BPD vs bipolar disorder discussions, because when both conditions are present, diagnosis and treatment can become more complex. Proper evaluation and a thorough assessment are essential to ensure effective care.
Is BPD Worse Than Bipolar Disorder?
Neither condition is inherently worse. They are simply different. Both BPD and bipolar disorder can significantly affect daily life, relationships, and overall wellbeing. Each comes with its own challenges, and severity can vary from person to person. Having either condition or both requires proper support and treatment. Understanding the differences and seeking professional care is key to managing symptoms effectively.
Conclusion
Mental health conditions like BPD and bipolar disorder are often misunderstood, and that misunderstanding can make an already difficult experience even harder. By understanding the key differences between borderline and bipolar disorder, individuals, families, and caregivers can approach these conditions with greater clarity, compassion, and confidence. While both conditions present unique challenges, proper diagnosis, treatment, and support can help manage symptoms, improve relationships, and lead to more balanced, fulfilling lives.

